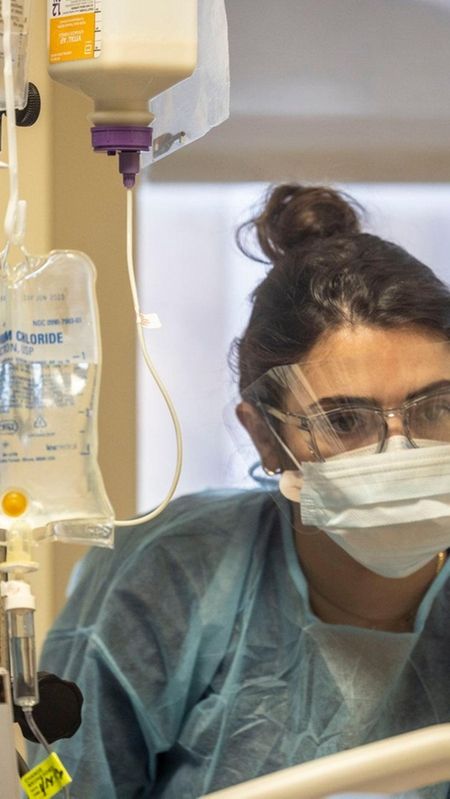
Newsday journalists David Olson, Faith Jessie and Alejandra Villa Loarca spent Jan. 13 inside Long Island Jewish Medical Center in New Hyde Park for an up-close look at the COVID-19 surge, which has been fueled by the omicron variant.
Long Island Jewish Medical Center nurse Julia Jozefowski sat outside the room of an unvaccinated COVID-19 patient in her 30s, monitoring the ECMO machine that was removing her blood, adding oxygen and pumping the blood back into her body.
Jozefowski said she sometimes ponders a different reality. In it, the critically ill patients she's caring for, like the woman struggling to survive, are inoculated and likely never would have been hospitalized, much less ended up in intensive care.
"It can make you emotional at times when you would do anything for this patient … you push yourself so hard to give these people a chance," she said. "It’s hard if you do take that moment to think about if something so much easier could have been done, [like] getting the vaccine."
Like other hospitals across the region, Long Island Jewish in New Hyde Park has been enduring a third major COVID-19 wave. Unlike the ones last winter and in spring 2020, this time almost all patients had access to a vaccine that is highly effective at preventing hospitalization.

Newsday spent Jan. 13 inside the Northwell Health hospital at around the peak of its omicron-fueled surge.
Nearly two years into COVID-19, health care workers are exhausted by the roller coaster nature of a pandemic that in the past few weeks has sent hundreds more coronavirus patients into the hospital. Hundreds of employees have been out sick with the virus, with those remaining sometimes working long hours to help fill the void. Many elective surgeries were postponed to ensure there were enough beds and staffing.
What to know
Omicron led to a surge in COVID-19 patients at Long Island Jewish Medical Center, and in staff out sick with the virus, but the impact on the hospital was far less intense than in spring 2020.
The large majority of coronavirus patients — especially severely ill ones — are unvaccinated, leading to some frustration among doctors, who view COVID-19 as largely a "preventable disease."
The less virulent effect of omicron in many people, as well as two years of experience treating coronavirus patients and improvements in treatment, have helped halve the amount of time COVID-19 patients stay in the hospital.
There are some positive signs. Confirmed COVID-19 cases on Long Island have fallen 80% in two weeks, according to state data, and hospitalizations at Long Island Jewish and throughout the region are dropping as well, although not as sharply. Patients have tended to be less sick than in previous waves. And health care workers are armed with experience and treatments they didn’t have then.
 'I thought we were kind of out of it'
'I thought we were kind of out of it'
 'I thought we were kind of out of it'
'I thought we were kind of out of it'The region’s high vaccination rates prevented a "very difficult" COVID-19 surge from being far worse, said the hospital’s executive director, Dr. Michael Gitman.
"I would imagine if we weren’t vaccinated, January 2022 would feel very similar to March 2020," he said.
Even so, some employees were surprised by how much hospitalizations had increased and how many health care workers were infected because of the surge.
"I thought we were kind of out of it, because we had the vaccine out and everyone was doing well," said Diana Tarello-Ketterer, a labor and delivery nurse. "And then it just kind of hit us like a tidal wave."
All employees are vaccinated, and many have received booster shots. Boosters lessen the chance of infection, but they don't eliminate it, especially with the highly contagious omicron variant, which was first detected in South Africa in November. But vaccination greatly reduces the risk of severe illness, even with omicron.
Long Island Jewish medical director Dr. Richard Schwarz said frustration among employees with unvaccinated patients is not uncommon.
"There’s no question that many people are irritated at all this preventable disease," Schwarz said, although he quickly added, "That’s a conversation for outside."

Dr. Mangala Narasimhan checks on a patient inside the medical intensive care unit at Long Island Jewish Medical Center in New Hyde Park on Tuesday. Credit: Newsday/Alejandra Villa Loarca
"When they come in and they’re patients, we’re professionals, we take care of our patients, we do what we’ve got to do," he said. "We take care of them and try not to be judgmental. If you ask me what I think about it when we have cocktails, I may say something different."
There were 275 COVID-19 patients on Jan. 13, slightly down from the omicron-era peak of 281 the day before, but nearly triple the 99 on Christmas Day. It was the highest number of COVID-19 patients in the 19-hospital Northwell system. The number had dropped to 229 by Tuesday morning.
There were 630 admitted patients on Jan. 13, Gitman said. The hospital typically has 583 inpatient room beds, so some patient rooms were doubled-up, and 13 admitted patients that morning were in the emergency department awaiting inpatient beds, he said.
But, Schwarz said, "This is nothing like we dealt with in 2020. In 2020, we had 900 patients, of whom 800 were COVID-positive."
This time, there were no lines of beds of COVID-19 patients in the endoscopy and post-anesthesia units, as there were nearly two years ago. There are no refrigerated trailers outside to hold patients who had died in such high numbers in 2020 that the hospital morgue and area funeral homes didn't have space for them.
Far fewer COVID-19 patients are desperately ill this winter. In spring 2020, 20% to 25% of coronavirus patients were in intensive care, Schwarz said.
On Jan. 13, there were 10 COVID-19 patients in intensive care, about eight on ventilators. In April 2020, there was a peak of more than 160 people on ventilators, said Sandra Lindsay, director of patient care services for the medical intensive care unit and a registered nurse.

A team of doctors and nurses checks on a patient in the medical intensive care unit at Long Island Jewish Medical Center in New Hyde Park on Tuesday. Credit: Newsday/Alejandra Villa Loarca
Nearly 340 people died of COVID-19 at Long Island Jewish in April 2020, and 88 died in January 2021. As of Tuesday morning, 22 had died this month, and 42 died in December. The effect of increased cases and hospitalizations typically is not seen in death numbers until days or weeks later.
Although omicron is on average less severe than the delta variant, that doesn’t mean it is that way for everyone, especially for unvaccinated people with chronic illnesses, said Lindsay, a Port Washington resident who on Dec. 14, 2020, became the first person in the United States to receive a COVID-19 vaccine after it was federally authorized.
"Getting COVID on top of a chronic condition is a recipe for disaster," she said.
All 10 COVID-19 intensive care patients Jan. 13 were unvaccinated. The few fully vaccinated COVID-19 patients in intensive care in the past few months had weakened immune systems because of organ transplants, lupus or other reasons, said Dr. Adey Tsegaye, director of intensivist medicine.
 Ventilators helping keep patients alive
Ventilators helping keep patients alive
 Ventilators helping keep patients alive
Ventilators helping keep patients aliveTsegaye looked into the room of one unconscious man connected to a web of tubes.
"We’re working toward getting him off the ventilator," Tsegaye said. "He’s doing well."
"Let me show you someone who is not doing well," she said as she walked down the hallway to the sound of a near-constant beep of machines that were helping keep patients alive.
"This one I’m worried about," Tsegaye said as she pointed to a man in his 50s facedown in his bed, a ventilator pumping oxygen into his body because his coronavirus-ravaged lungs could no longer do so alone.
"He spends 16 to 18 hours a day on his belly," to help increase oxygen levels, she said.
Even if the man survives, he could have long-term, perhaps lifelong, complications.
"When they get better, they have to learn how to walk again, learn how to eat again, once they have learned how to breathe again," Tsegaye said. "You’re fully dependent on us and then your family members for months, sometimes years."
More than a third of patients with COVID-19 at Long Island Jewish on Jan. 13 were fully vaccinated. But the large majority of the region’s residents are vaccinated, so an unvaccinated person with COVID-19 is far more likely to be hospitalized. Nationwide, unvaccinated adults are 16 times more likely to be hospitalized for COVID-19 than vaccinated adults, according to the Centers for Disease Control and Prevention.
Most vaccinated patients had medical conditions that put them at higher risk for severe COVID-19, Schwarz said.
In addition, on Jan. 13 about half the patients with COVID-19 entered the hospital for other reasons and tested positive upon admission, Schwarz said. COVID-19 exacerbates some health conditions, but it’s difficult to determine in which cases COVID-19 may have caused a condition to deteriorate enough to require hospitalization, Gitman said.
Guohua Quan, 34, of East Meadow, didn’t find out she was positive until she had a routine test before a C-section birth.
"I was freaking out the moment I heard I had a COVID-positive" result, Quan said as she sat in her hospital room chair two days after her baby Alice was born without COVID-19. She thought, " ‘Wait a second, I have no symptoms. I don’t have fever. I don’t have cough. I was working still until right before’ " going to the hospital.

Quan said she was grateful she was vaccinated, because it may have prevented her from getting seriously ill.
In the week ending Jan. 3, 25% of women in labor and delivery and postpartum tested positive, with a high of 22 positive results on Dec. 31, said Dr. Monique De Four Jones, associate chief of labor and delivery for Katz Women's Hospital, which is part of Long Island Jewish.
"At one point last week, from here down to the end of the door was all COVID-positive," Jones said as she gestured down a long hallway.
On Jan. 13, 13 women tested positive.
COVID-19 patients spend on average much less time in the hospital today than two years ago, Gitman said. In spring 2020, the average length of stay was 11.9 days, compared with six days now.
That’s in part because omicron often is less virulent, he said. In addition, Schwarz said, some patients are sent home early — or not admitted at all — if they can be safely cared for at home, with an oxygen monitor and with in-person or virtual visits from a health care professional, he said.
Two years of experience in treating coronavirus patients, and more available treatments, also have helped cut down hospitalization time.
"Unlike 2020, we’re not wasting our time doing a lot of things that don’t work," Schwarz said. "When [patients] first came in, we were doing hydroxychloroquine, we were doing all sorts of things that don’t work. We have a better idea now how to manage and how not to manage these patients. We’re not spinning wheels as we were in the beginning."
"We’re able to not be in a reactive mode," Lindsay said, "and be more proactive."
The paucity of non-COVID-19 patients in spring 2020 reflected how fearful people were of contracting the coronavirus then, Schwarz said. In recent months, the hospital has had an influx of patients who doctors believe delayed care earlier in the pandemic and now need treatment, he said.
In the emergency department, "We were seeing the complications of all that — patients who haven’t seen their doctors in months, who have been off medications, who missed a few [treatments of] dialysis and were now presenting to the emergency room, sicker than they normally would be," said Dr. Fred Davis, associate chair of emergency medicine.
 Avoiding hospital for fear of infection
Avoiding hospital for fear of infection
 Avoiding hospital for fear of infection
Avoiding hospital for fear of infectionThere are signs some people may be avoiding the hospital during the current surge because of fears of getting infected, or worries about overcrowding, Gitman said.
But the hospital segregates COVID-19 patients from non-COVID-19 ones, and the quality of care is the same as pre-surge, he said.
"Our patients should feel comfortable coming in for care," he said.
The hospital has postponed 25% of its surgeries — the ones considered non-urgent — to avoid a shortage of staffing or beds, Gitman said.
The other 75% include, for example, cancer surgeries.
"Things that we thought would lead to harm if it waited, we’re able to do," he said.
In the spring 2020 wave, nearly all surgeries were halted, because there was no room for them and the hospital worried about keeping surgical patients safe, Gitman said.
"There are people who certainly didn’t get surgeries in time," and diseases such as cancer may have progressed far enough that there were "in some of those cases a worse outcome," including death, he said.
This winter, the hospital never reached that point. The emergency department has seen a drop in overall patients since its omicron-era peak in late December, and a fall in the percentage who tested positive, from more than half to about a third, Helena Willis, senior director of patient care services and a registered nurse, said Jan. 13.
A spike in COVID-19 and non-COVID ambulance calls has abated, said Jackie Berman, a paramedic supervisor for Northwell.
 Hundreds of staff out sick
Hundreds of staff out sick
 Hundreds of staff out sick
Hundreds of staff out sickFewer staff also have been out recently. On Dec. 29, 370 of the hospital’s 5,500 employees were on a COVID-19-related quarantine, a number that dropped to 112 by Jan. 12.
"Staffing is good today, and our sick calls continue to decline, so that is great news," Pat Hermann, director of integrated staffing, said during a Jan. 13 COVID-19 "command center" video call of more than 100 hospital employees that was revived for the omicron surge.
"It does really feel like we’re reaching the beginning of the end," Schwarz said during the call.
Northwell, the state’s largest health care system, with 11 hospitals on Long Island, has used its size to mitigate the effect of staff absences by moving employees around hospitals, based on need, bringing in employees who typically are in ambulatory-care settings, and deploying employees from its own internal staffing agency, as well as contracting with outside agencies, Gitman said.
Even so, Tarello-Ketterer said, the two weeks beginning around Christmas Eve felt "like the hardest two weeks of my nine-year career, just because there were a lot of COVID-positive patients and a lot of COVID-positive staff members, and that combination just really hit us strong."
She recalled how starting Christmas Eve, "All of a sudden everybody seemed to be getting sick — all mild symptoms, which we were thankful for, but they still couldn’t work."
As a result, nurses were working extra shifts and staying late, she said.
Schwarz said, even with the outside help, staff in recent weeks have had to take care of more patients than they used to and "moved faster."
After two years of employees working "incredibly hard," burnout is a problem, and some likely left their jobs because of it, Gitman said. But, he said, hospital managers have encouraged employees to take time off, and the hospital is continuously hiring new nurses and other personnel.
Berman said that, during the surges, "It’s mentally draining. During the lulls, we kind of reset ourselves. We all kind of expected the winter to spike, so we mentally prepared ourselves. Now that we’re in the spike, you just put your head in the game and just keep going through it."
Photos and video by Newsday/Alejandra Villa Loarca