Long Island clinic to treat people with lingering health effects of COVID-19
A new Stony Brook Medicine clinic for people with long-term effects of COVID-19 aims to improve treatment for coronavirus survivors and lead doctors to better understand how the virus can wreak havoc on the body.
Many continue to struggle with illness or other health effects months after contracting the virus. Heart, kidney and lung problems, fatigue and persistent cough are among the most common maladies, said Dr. Margaret McGovern, Stony Brook’s vice president for health system clinical programs and strategy.
But with the disease so new, doctors "really don’t know what we could call the natural history of a post-COVID infection: What is it that happens at six months, one year, 18 months?" said McGovern, who is helping create the clinic to assist Long Islanders. "It’s not going to be the same for every patient. That has to be learned."
The Stony Brook Medicine Post COVID Clinic, set to open the week of Nov. 16, will use existing space at Stony Brook’s Advanced Specialty Care center in Commack. It will start out as once a week, with 25 to 30 patients seen in a day, but "if we find that’s not sufficient to meet demand, we can add days," McGovern said.
Patients will have access to a battery of specialists, including cardiologists, neurologists and lung, kidney, and vascular specialists, as well as psychiatrists and psychologists, who can address the mental health impacts of the disease, she said. Many patients with long-term effects of the coronavirus have multiple problems, so they will need to see more than one specialist.
"You have a whole team of specialists discussing every patient, bringing together all the information, trying to understand the whole picture of what the patient is going through," McGovern said.
The virus affects patients in different and unpredictable ways, and the team approach facilitates individualized care, said Dr. Apostolos K. Tassiopoulos, chief of vascular and endovascular surgery at Stony Brook.

Dr. Sritha Rajupet,director of Population-Based Health Initiatives and Primary Care Lead for the Stony Brook Medicine Post COVID Clinic in Commack, Nov. 5, 2020. Credit: Johnny Milano
Specialists will confer to make sure that a treatment that helps address one condition does not cause unintended negative effects for another, he said.
Patients can opt to visit all the relevant specialists in Commack, or see some doctors elsewhere, McGovern said.
The Stony Brook program may be the first of its kind on Long Island.
The Mount Sinai Health System in May created a Center for Post-COVID Care in Manhattan that, like Stony Brook, offers an array of specialists.
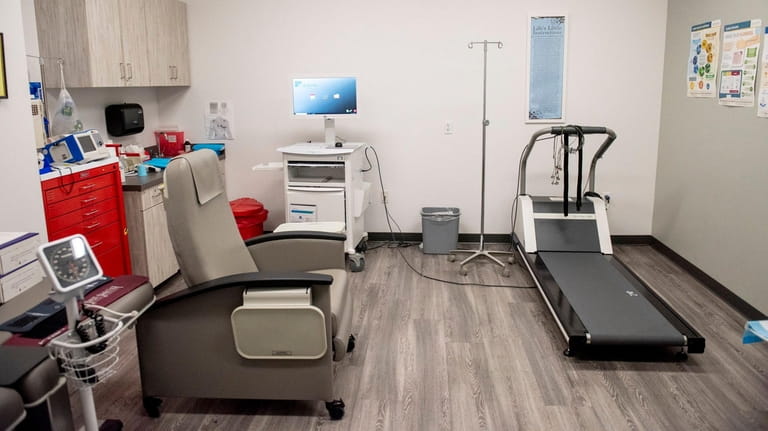
The Stress Test room at Stony Brook Medicine's Advanced Specialty Care facility in Commack for patients who are still dealing with lingering complications from COVID-19, Nov. 5, 2020. Credit: Johnny Milano
At St. Charles Hospital, a Catholic Health Services of Long Island hospital in Port Jefferson, a post-coronavirus rehabilitation program began in September with a focus on medically supervised physical therapy and strength training.
Dr. Sritha Rajupet, the primary care lead for the Stony Brook clinic and Stony Brook Medicine’s director of population-based health initiatives, will help coordinate each patient's care in Commack.
Rajupet and other doctors may become clinic patients’ primary care physicians, if they don’t already have one. But the goal is not to supplant existing primary care doctors, Rajupet said. Physicians at the clinic can learn more about the patients by talking with those doctors, and clinic physicians can then share their COVID-19 knowledge with patients’ longtime doctors, she said.
A big benefit of the clinic is that doctors there will build up expertise in COVID-19 by treating patients and discussing cases with other physicians, and they’ll be responsible for keeping up with COVID-19 studies and developments from around the world, McGovern said.
"They’ll become our local experts on this disorder and its long-term impacts, and a resource regionally for the other physicians out there who no doubt will see patients who have had COVID, but won’t invest the time and energy to keep up with what’s the latest thinking," McGovern said.
Dr. Hal Skopicki, chief of cardiology at Stony Brook, said that, if a patient at the clinic already has a cardiologist, he can work with that cardiologist on a long-term treatment plan.
"The cardiologist now knows how to look at all the other COVID-positive patients they have coming into their practice," he said.
Many patients recovering from COVID-19 have scarring and inflammation in the heart that puts them at higher risk for coronary disease and heart attacks, Skopicki said.
He and other cardiologists at the clinic will monitor patients to ensure the inflammation isn’t increasing and look for signs of worsening heart disease, he said. They’ll also "identify which patients need to be seen regularly and frequently, and which patients need to be seen regularly and not as frequently, and personalize that care," he said.
The inflammation triggered by COVID-19 also can cause blood clots, Tassiopoulos said. Blood clots can be helpful if, for example, the body activates coagulation to prevent excess bleeding from an injury, he said. But they are harmful if they prevent blood from flowing through healthy blood vessels, which is what occurs with some COVID-19 patients, he said. As a result, some post-coronavirus patients have chronic swelling that they may have the rest of their lives, and, later, they could have lifelong skin discoloration, he said.
McGovern said Stony Brook will ask clinic patients for permission to collect data on them. That will allow Stony Brook to better study the long-term impacts of a disease whose trajectory is still uncharted.
"No one knows the answers yet," she said.

